
menu


Snoring results from an often-complex multi-facial problem that can be affected by one or more anatomical factors. For most sufferers, snoring is caused by the vibration of the muscular roof of the mouth, also known as the soft palate. For others, snoring is worsened by an obstruction of the nasal passage. An enlarged uvula, tonsils, and the base of the tongue can also contribute to the problem.
There is no reason to be embarrassed about snoring, or to feel alone. Snoring is a common problem, with 90 million Americans suffering from the condition. While snoring can have a negative impact on your personal life, it can also negatively affect your health, and should therefore be taken seriously. Daytime drowsiness, decreased libido and energy, and even depression can all result from snoring. More serious problems such as an increased risk of heart attacks and stroke, type 2 diabetes, weight gain, and high blood pressure can also result from habitual snoring.
Do not wait to have your snoring problem examined. Our Doctors can help you determine the cause and a course of treatment for your snoring, which may help save your relationships- and your life!
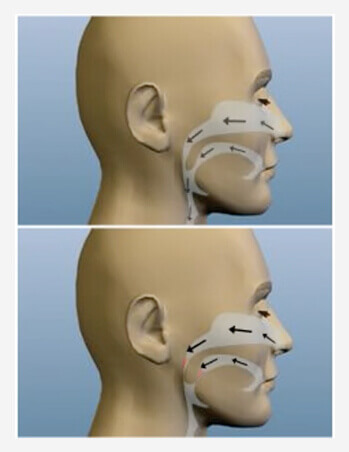
People with obstructive sleep apnea (OSA) have disrupted sleep and low blood oxygen levels. When obstructive sleep apnea occurs, the tongue is sucked against the back of the throat. This blocks the upper airway and airflow stops. When the oxygen level in the brain becomes low enough, the sleeper partially awakens, the obstruction in the throat clears, and the flow of air starts again, usually with a loud gasp.
Repeated cycles of decreased oxygenation lead to very serious cardiovascular problems. Additionally, these individuals suffer from excessive daytime sleepiness, depression, and loss of concentration.
The first step in treatment resides in recognition of the symptoms and seeking appropriate consultation. Our ENT doctors offer consultation and treatment options.
In addition to a detailed history, the doctors will assess the anatomic relationships with a flexible fiber-optic camera. To confirm the amount of cardiovascular compromise and decreased oxygenation levels, a sleep study may be recommended to monitor an individual overnight.
There are several treatment options available. An initial treatment may consist of using a CPAP machine that delivers pressurized air through a mask to limit obstruction at night. One of the surgical options is an uvulo-palato-pharyngo-plasty (UPPP), which is performed in the back of the soft palate and throat.
OSA is a very serious condition that needs careful attention and treatment. Most major medical plans offer coverage for diagnosis and treatment.
Obstructive sleep apnea (OSA) is a serious health condition characterized by a repetitive stopping or slowing of breathing that can occur hundreds of times during the night. This often leads to poor quality sleep and excessive daytime sleepiness. Risks of untreated sleep apnea include high blood pressure, stroke, heart disease, and motor vehicle accidents. It is estimated that 1 in 5 Americans have at least mild OSA.
A variety of surgical and non-surgical options are available for the treatment of snoring and sleep apnea. Medical options include positive pressure (i.e. CPAP), oral appliances, and weight loss. Many of these treatment options depend on regular, long-term adherence to be effective. In patients having difficulty with other treatments, surgical procedures for the nose and throat can be a beneficial alternative. Surgical therapy can also be effective when used as an adjunct to improve tolerance and success with CPAP or an oral appliance.
Increased nasal congestion has been shown to cause or contribute to snoring, disrupted sleep, and even sleep apnea. It is also a leading cause of failure of medical treatments for OSA, such as CPAP or an oral appliance. Nasal obstruction may result from many causes including allergies, polyps, deviated septum, enlarged adenoids, and enlarged turbinates.
Medical treatment options, such as a nasal steroid spray or allergy management, may be helpful in some patients. Structural problems, such as a deviated septum, often benefit from surgical treatment.
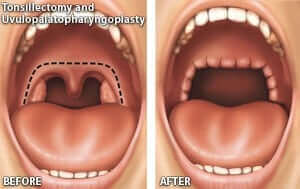
In many patients with OSA, airway narrowing and collapse occurs in the area of the soft palate (back part of the roof of the mouth), tonsils, and uvula. The specific type and combination of procedures that are indicated depend on each individuals unique anatomy and pattern of collapse. Therefore the procedure selection and surgical plan must be customized to each patient. In general, these procedures aim to enlarge and stabilize the airway in the upper portion of the throat.
The surgery is performed in an operating room under general anesthesia, either as an outpatient or with an overnight hospital stay. The recovery varies depending on the patient and the specific procedures performed. Many patients return to school/work in approximately one week and return to normal diet and activity at two weeks. Throat discomfort, particularly with swallowing, is common in the first two weeks and usually managed with medications for pain and inflammation. Risks include bleeding, swallowing problems, and anesthesia complications, although serious complications are uncommon.
The tonsils and adenoids may be the sole cause of snoring and sleep apnea in some patients, particularly children. In children, and in select adults, with OSA and enlarged tonsils/adenoids, tonsillectomy/adenoidectomy alone can provide excellent resolution of snoring, sleep apnea, and associated symptoms.
The lower part of the throat is also common area of airway collapse in patients with OSA. The tongue base may be larger than normal, especially in obese patients, contributing to blockage in this area. The tongue may also collapse backward during sleep as the muscles of the throat relax, particularly when some patients sleep on their back. The epiglottis, or upper part of the voice box, may also collapse and contribute to airway obstruction.
Multiple procedures are available to reduce the size of the tongue base or advance it forward out of the airway. Other procedures aim to advance and stabilize the hyoid bone which is connected to the tongue base and epiglottis. A more recent technology involves implantation of a pacemaker for the tongue (hypoglossal nerve stimulator) which stimulates forward contraction of the tongue during sleep. As with palatal surgery, the most appropriate type of procedure varies from one individual to another, and is primarily determined by each patients anatomy and pattern of obstruction.
The procedures are done under general anesthesia, often with overnight hospital observation. Recovery and risks vary depending on the procedure(s) performed, but are generally similar to procedures in the upper throat.
For the most part, the above procedures involve surgical enlargement and stabilization inside the airway. For some patients, particularly those with developmental or structural changes of the jaw or other facial bones, surgical or orthodontic procedures on the bones of the face, jaw, or hard palate (roof of the mouth) may be beneficial.
Orthodontic procedures to widen the palate (palatal or maxillary expansion) may be useful treatment options in some pediatric patients. Maxillomandibular advancement surgery includes a number of procedures designed to move the upper jaw (maxilla) and/or lower jaw (mandible) forward, thus opening the upper and/or lower airway, respectively. Although full maxillomandibular advancement surgery can provide effective enlargement and stabilization of the airway, the potential benefits must be cautiously weighed against the potential increased risks of complications, longer recovery, and changes in the cosmetic appearance of the face.
Surgery is an effective and safe treatment option for many patients with snoring and sleep apnea, particularly those who are unable to use or tolerate CPAP. Proper patient and procedure selection is critical to successful surgical management of obstructive sleep apnea.
Talk to your Ear, Nose and Throat doctor for a complete evaluation and to learn what treatment may be best for you.
Please refer to After Sleep Apnea Surgery for post-operative instructions.
Obstructive sleep apnea is a serious condition that affects 4-9% of the United States population. People with OSA have disrupted sleep and low blood oxygen levels. When obstructive sleep apnea occurs, the tongue is sucked against the back of the throat. This blocks the upper airway and airflow stops. When the oxygen level in the brain becomes low enough, the sleeper partially awakens, the obstruction in the throat clears, and the flow of air starts again, usually with a loud gasp.

Repeated cycles of decreased oxygenation lead to very serious cardiovascular problems. Additionally, these individuals suffer from excessive daytime sleepiness, depression, and loss of concentration.
To diagnose sleep apnea and other sleep disorders, a sleep study at an overnight sleep lab has traditionally been recommended. However, portable sleep monitoring devices have recently emerged to help identify disruptive sleep patterns without sacrificing your time or comfort.
Home sleep studies allow our ENT Doctors to monitor your sleep patterns in the comfort of your own home, and without interrupting your normal nightly routine. The home sleep study device is generally worn on your chest while finger probes connected to the device gather your data and vital signs. The information is stored on a removable memory card and downloaded for the doctors to analyze. The doctors will then be able to recommend an appropriate treatment method for you.

Continuous Positive Airway Pressure (CPAP) is a treatment option for patients suffering from obstructive sleep apnea (OSA). When OSA occurs, the tongue is sucked against the back of the throat. This blocks the upper airway and airflow stops. When the oxygen level in the brain becomes low enough, the sleeper partially awakens, the obstruction in the throat clears, and the flow of air starts again, usually with a loud gasp.
The CPAP treatment is generally offered to patients with moderate to severe sleep apnea, and involves wearing a mask placed on the nose and/or mouth during sleep, which helps keep the airways open during. The mask is attached to a machine that delivers a continuous stream of compressed air.
The CPAP mask must be worn nightly for at least 4 hours in order to be effective.
When used properly, CPAP is a highly effective way to treat OSA. It reduces the risk of heart problems such as heart failure, decreases daytimes sleepiness, and may lower blood pressure both when in use and during waking hours.
Unfortunately, some users find the mask uncomfortable or inconvenient, and reduce use without consulting their doctor. Other patients may experience dry mouth, or complain that the noise produced by the machine actually makes sleep more difficult. Our ENT Doctors will help you determine the best method of treatment for your OSA.
Please refer to Sleep Apnea and Home Sleep Study for more information.